A Quick Refresher on LABAs and SABAs
Most common short-acting beta-agonist (SABA) medications are albuterol and levalbuterol. Similarly, the most common long-acting beta-agonist (LABA) medications are salmeterol and olodaterol. These medications are used to help alleviate the many symptoms of asthma and chronic obstructive pulmonary disease (COPD).
SABAs are in the beta-2 adrenergic agonist bronchodilators family. Their onset of action is roughly seen in 15 minutes and lasts for about four to six hours. The common side effects of SABA medications are fast heart rate and tremors. They are used as rescue medications to relax and open the airway passages in the lungs. Consequently, SABAs resolve symptoms such as shortness of breath, cough, and wheezing. The main chemical structure difference between albuterol and levalbuterol is that albuterol is made up of R-albuterol (active form) and S-albuterol (inactive form), whereas levalbuterol is composed of R-albuterol (active form). Both albuterol and levalbuterol are approved for ages four years and older and they are used to treat or prevent bronchospasms. Usually, they are dosed at one to two puffs by mouth every four to six hours. If using albuterol for exercise-induced bronchospasm, it’s important to instruct patients to take their dose 15 to 30 minutes before starting exercise.
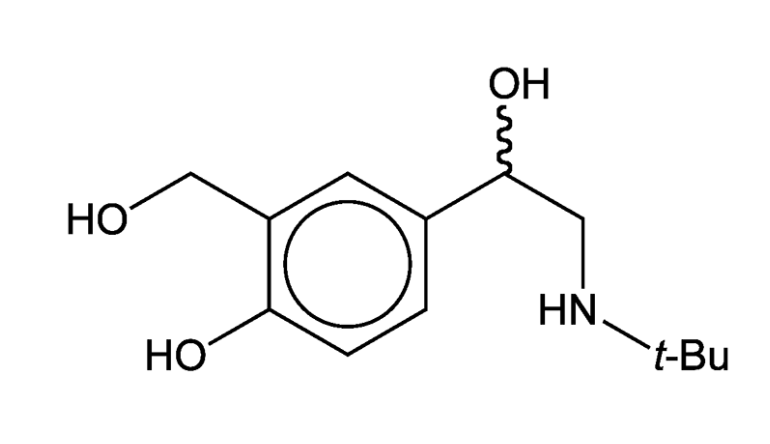
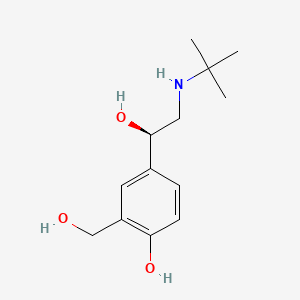
Image 1: Chemical Structure of Albuterol
LABA medications are in the beta-2 adrenergic agonist bronchodilators family as well, but are seen in chronic settings compared to SABA medications. LABAs are commonly used in asthma and COPD. Their effects are seen in about 30 minutes and their duration lasts for about 12 to 24 hours. Salmeterol can be used to treat asthma, but the patient must be on an inhaled corticosteroid at the same time. Salmeterol is also used to prevent exercise-induced bronchospasm and is indicated for maintenance treatment of COPD. The common dose is usually one inhalation by mouth twice daily. On the other hand, olodaterol is considered ultra-LABA compared to salmeterol because of its effects lasting closer to 24 hours. Olodaterol is only indicated for COPD, unlike all the other medications we discussed thus far. Commonly, olodaterol is dosed at two inhalations by mouth daily. It is also important to note is that salmeterol and olodaterol are available in combination inhalers.
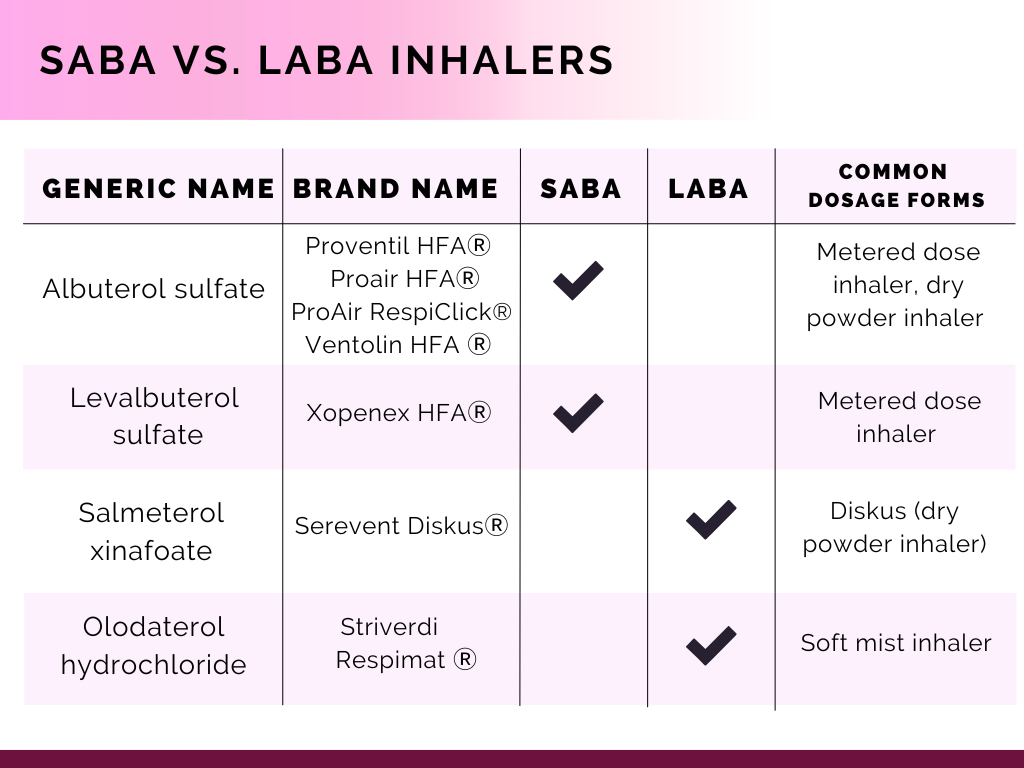
The SABAs discussed are available in metered dose inhalers or dry powder inhalers. The LABAs mentioned are available in Diskus inhalers or soft mist inhalers. The adverse effects are dependent on the dosage form. Lastly, it is crucial to educate patients on proper usage of the inhalers, such as priming, storage, and missed doses in counseling settings.
Keep in mind that SABAs have short-acting properties and LABAs have long-acting properties. One way to remember the effect of these inhalers is that SABAs start with an “S” which can be associated with short-acting properties, and LABAs start with an “L” which can be associated with long-acting properties. Even though this quick refresher does not list of all SABAs and LABAs, we have provided the most common medications from these classes to help with these educational concepts. If using a more in-depth study approach, mnemonics, flashcards, and practice exams are always a helpful way to master even more comprehensive material.
-Dagmara Zajac, 2022 RxPharmacist Intern
References:
- Albuterol. American Chemical Society. Available at: https://www.acs.org/content/acs/en/molecule-of-the-week/archive/a/albuterol.html (Accessed: October 10, 2022).
- Ameredes BT, Calhoun WJ. Levalbuterol versus albuterol. Curr Allergy Asthma Rep. 2009;9(5):401-409. doi:10.1007/s11882-009-0058-6
- Hsu E, Bajaj T. Beta 2 Agonists. [Updated 2022 Jun 23]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK542249/
- Levalbuterol. National Center for Biotechnology Information. PubChem Compound Database. U.S. National Library of Medicine. Available at: https://pubchem.ncbi.nlm.nih.gov/compound/Levalbuterol#section=Structures (Accessed: October 10, 2022).
- Levalbuterol oral inhalation: Medlineplus Drug Information. MedlinePlus. U.S. National Library of Medicine. Available at: https://medlineplus.gov/druginfo/meds/a603025.html (Accessed: October 10, 2022).
- Lanser, C. (2021) Beta-agonists (sabas and labas), AlphaNet. Available at: https://www.alphanet.org/living-with-alpha-1/medications-for-alpha-1/beta-agonists/ (Accessed: October 10, 2022).
- ProAir HFA (albuterol) [prescribing information]. Parsippany, NJ: Teva Pharmaceuticals USA, Inc; August 2020.
- Serevent Diskus (salmeterol) [prescribing information]. Research Triangle Park, NC: GlaxoSmithKline; February 2022.
- Striverdi Respimat (Olodaterol) [prescribing information]. Ridgefield, CT: Boehringer Ingelheim Pharmaceuticals Inc; November 2021.
- Xopenex HFA (levalbuterol) [prescribing information]. Marlborough, MA: Sunovion Pharmaceuticals Inc; February 2017.
A Quick Refresher on LABAs and SABAs Read More »
